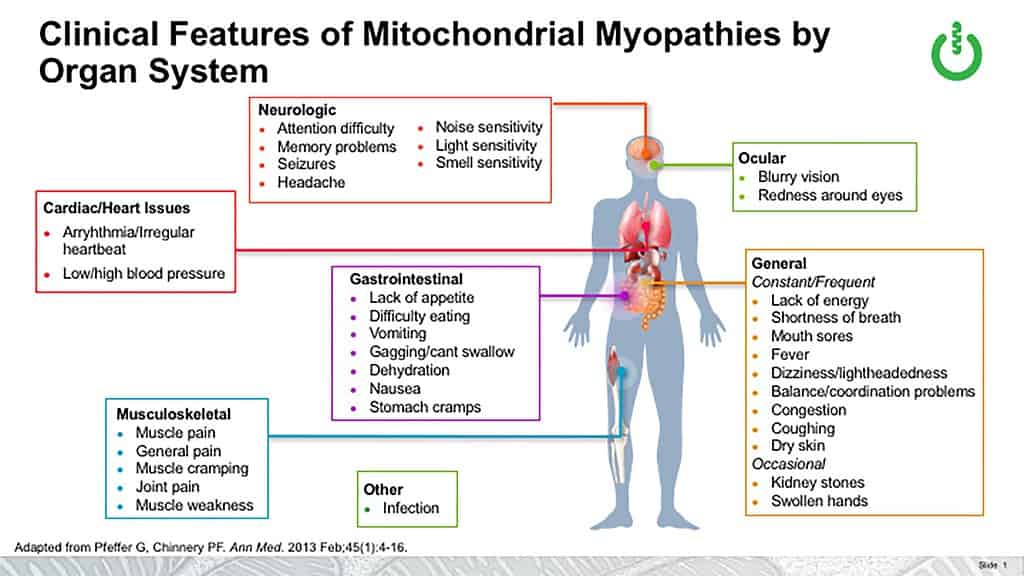
MitochondrialRelated to the mitochondria. diseases are a varied group of disorders characterized by impaired energy production. The symptoms of mitochondrial disease can arise in any organ at any age. Some symptoms are hallmarks of mitochondrial disease and are called “red flag” symptoms.
Neurologic
- Cerebral stroke-like lesions in a nonvascular pattern (brain lesions that do not appear like a regular stroke on imaging)
- Basal gangliaA group of structures in the base of the brain. That are primarily responsible for motor control, motor learning, executive function, behavior, and emotions. disease (physical dysfunction, such as would occur with Parkinson’s disease)
- Encephalopathy (brain disease) recurrent or with low/ moderate dosing of valproate (a medicine used to treat epilepsy, bipolar disease, and migraines)
- Neurodegeneration (the progressive loss of structure or function of neurons, including death of neurons)
- Epilepsia partialis continua (recurrent epileptic seizuresEpisodes of abnormal electrical activity in the brain. that affect specific areas and recur every few seconds or minutes for extended periods)
- Myoclonus (jerky contraction of groups of muscles)
- AtaxiaImpaired coordination of voluntary muscle movements. Manifestations can include, among others, slurred speech, poor balance, unsteady walking, falling, and involuntary eye movements (nystagmus). Usual... (loss of control of body movements)
- MRI findings consistent with Leigh disease (in basal ganglia or brain stem)
- Characteristic magnetic resonance spectrometry (MRS) peaks
Cardiovascular
- Hypertrophic cardiomyopathyAn abnormal condition of the heart muscle. Occurs in some kinds of mitochondrial disease. with rhythm disturbance (thick heart muscle that can lead to irregular heartbeat)
- Unexplained heart block in a child
- Cardiomyopathy with lactic acidosis (build up of lactic acid in the body)
- Dilated cardiomyopathy with muscle weakness
- Wolff-Parkinson-White arrhythmia (a disorder of the heart’s electrical system that can cause fast heartbeat, palpitations, shortness of breath, and fainting)
Ophthalmologic
- Retinal (the back of the eye) degeneration with signs of night blindness, color-vision deficits, decreased visual acuity, or pigmentary retinopathy
- OphthalmoplegiaParalysis or weakness of the eye muscles. A common symptom in some kinds of mitochondria disease paresis (weakness or paralysis of eye muscles)
- Fluctuating, dysconjugate eye movements (eyes not moving together)
- PtosisDrooping of the upper eyelid to some degree over the eye, in one or both eyes. A common symptom of mitochondrial disease. (droopy upper eyelid)
- Sudden or insidious-onset optic neuropathy/atrophy (damage to the optic nerve)
Gastroenterological
- Unexplained or valproate-induced liver failure
- Severe dysmotility (digestive tract muscles are impaired; food does not move through the system)
- Pseudo-obstructive episodes (problem with gut motility that mimics an obstruction)
Other
- A newborn, infant, or young child with unexplained hypotonia (low muscle tone), weakness, failure to thrive, and a metabolic acidosis (particularly lactic acidosis)
- Exercise intolerance that is not in proportion to weakness
- Hypersensitivity to general anesthesia
- Episodes of acute rhabdomyolysisBreakdown of muscle tissue, releasing muscle fiber contents into the blood, with complex and potentially fatal consequences. Muscle contents are harmful to the kidney; rarely, permanent muscle damage ... (death of muscle fibers, which are then released into the blood stream)










